Understanding Psoriasis On Feet: Symptoms, Causes, Treatments, And More
Psoriasis on feet is a common yet often misunderstood skin condition that affects millions of people worldwide. It is a chronic autoimmune disorder that causes the rapid buildup of skin cells, leading to thick, scaly patches on the skin. When psoriasis develops on the feet, it can cause discomfort, pain, and even difficulty walking. Understanding the condition and its triggers is the first step toward managing it effectively.
Living with psoriasis on feet can be challenging, but with the right treatment and lifestyle adjustments, many individuals find relief and improve their quality of life. In this article, we will delve into the causes, symptoms, and treatments for psoriasis on feet, providing actionable insights for those affected by this condition.
This guide aims to equip you with comprehensive information about psoriasis on feet, helping you make informed decisions about managing your symptoms. Whether you're newly diagnosed or seeking better ways to control flare-ups, this article will provide valuable resources and expert advice.
Table of Contents
- What is Psoriasis on Feet?
- Symptoms of Psoriasis on Feet
- Causes of Psoriasis on Feet
- Diagnosing Psoriasis on Feet
- Treatment Options for Psoriasis on Feet
- Lifestyle and Home Remedies
- Complications of Psoriasis on Feet
- Preventing Psoriasis Flare-Ups
- Emotional Impact of Psoriasis
- Conclusion
What is Psoriasis on Feet?
Psoriasis is a long-lasting autoimmune condition that primarily affects the skin. When it occurs on the feet, it can lead to red, inflamed patches, thickened skin, and silvery scales. Unlike other forms of dermatitis, psoriasis is not contagious, but it can significantly impact daily activities such as walking or wearing shoes.
This condition arises due to an overactive immune system that accelerates the life cycle of skin cells. As a result, dead skin cells accumulate on the surface, forming plaques. Psoriasis on feet often affects the soles, heels, and toes, causing discomfort and sometimes embarrassment.
While there is no cure for psoriasis, various treatments and lifestyle changes can help manage symptoms and reduce flare-ups. Understanding the condition is key to effective management.
Symptoms of Psoriasis on Feet
The symptoms of psoriasis on feet can vary from person to person, but common signs include:
- Thick, red patches on the soles or heels
- Scaly, silvery skin
- Pain or tenderness in the affected areas
- Cracking or bleeding skin
- Swelling and stiffness in the joints (if psoriatic arthritis is present)
Some individuals may also experience itching or burning sensations. In severe cases, psoriasis on feet can lead to difficulty walking or standing for extended periods.
Causes of Psoriasis on Feet
The exact cause of psoriasis remains unknown, but research suggests that it is linked to genetic and environmental factors. Psoriasis on feet occurs when the immune system mistakenly attacks healthy skin cells, triggering rapid cell growth.
Factors that may contribute to the development of psoriasis include:
- Genetic predisposition
- Stress
- Infections, such as strep throat
- Injury to the skin (cuts, burns, or sunburns)
- Smoking and excessive alcohol consumption
While psoriasis is not contagious, it tends to run in families, suggesting a hereditary component.
Diagnosing Psoriasis on Feet
Diagnosing psoriasis on feet typically involves a physical examination by a dermatologist or healthcare professional. They may ask about your medical history, symptoms, and any family history of psoriasis. In some cases, a skin biopsy may be performed to rule out other conditions like eczema or fungal infections.
Early diagnosis is crucial for effective treatment. If you notice persistent redness, scaling, or discomfort on your feet, consult a healthcare provider promptly.
Treatment Options for Psoriasis on Feet
Topical Treatments
Topical treatments are often the first line of defense against psoriasis on feet. These include creams, ointments, and lotions that can be applied directly to the affected areas. Common topical treatments include:
- Corticosteroids to reduce inflammation
- Vitamin D analogs to regulate skin cell growth
- Salicylic acid to remove scales
These treatments are generally safe and effective for mild to moderate cases of psoriasis.
Oral Medications
For more severe cases, oral medications may be prescribed. These include:
- Methotrexate to slow skin cell production
- Cyclosporine to suppress the immune system
- Biologics, which target specific parts of the immune system
Oral medications require close monitoring by a healthcare provider due to potential side effects.
Light Therapy
Light therapy, also known as phototherapy, involves exposing the skin to controlled amounts of ultraviolet (UV) light. This treatment can help reduce inflammation and slow the growth of skin cells. Light therapy is often used in combination with topical or oral treatments for optimal results.
Lifestyle and Home Remedies
In addition to medical treatments, certain lifestyle changes and home remedies can help manage psoriasis on feet:
- Keep your feet moisturized to prevent dryness and cracking
- Wear comfortable, breathable shoes to reduce irritation
- Avoid triggers such as stress, smoking, and alcohol
- Soak your feet in warm water with Epsom salt or oatmeal
- Exercise regularly to improve circulation and reduce stress
These simple steps can complement medical treatments and improve overall skin health.
Complications of Psoriasis on Feet
Untreated or poorly managed psoriasis on feet can lead to several complications, including:
- Infections due to cracked or broken skin
- Psoriatic arthritis, which causes joint pain and stiffness
- Difficulty walking or standing
- Emotional distress and social withdrawal
Seeking prompt treatment and regular follow-ups with a healthcare provider can help prevent these complications.
Preventing Psoriasis Flare-Ups
While psoriasis flare-ups cannot always be avoided, certain measures can help minimize their frequency and severity:
- Maintain a healthy diet rich in fruits, vegetables, and omega-3 fatty acids
- Stay hydrated and avoid dehydration
- Protect your skin from injury or trauma
- Practice stress management techniques such as meditation or yoga
By identifying and avoiding personal triggers, you can better control your psoriasis symptoms.
Emotional Impact of Psoriasis
Psoriasis on feet can have a significant emotional impact, leading to feelings of self-consciousness, anxiety, or depression. It is essential to address these emotional challenges alongside physical symptoms. Support groups, counseling, and open communication with loved ones can provide valuable emotional support.
Remember that you are not alone in your journey. Many individuals with psoriasis lead fulfilling lives with the right treatment and support system.
Conclusion
Psoriasis on feet is a challenging condition, but with the right knowledge and resources, it can be effectively managed. From understanding the causes and symptoms to exploring treatment options and lifestyle changes, this guide aims to empower you to take control of your health.
We encourage you to share your experiences and insights in the comments section below. Additionally, consider exploring other articles on our website for more information about psoriasis and related topics. Together, we can raise awareness and improve the quality of life for those affected by psoriasis.
References:
- National Psoriasis Foundation
- American Academy of Dermatology
- World Health Organization
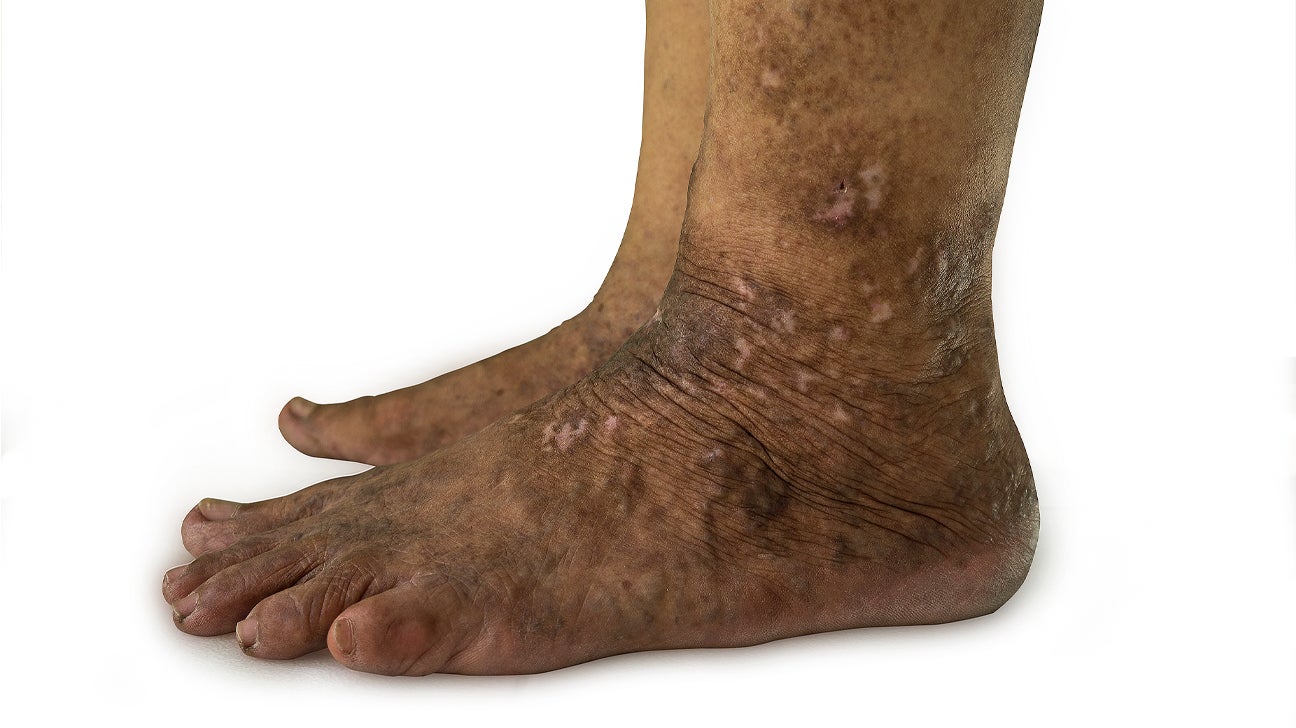
Psoriasis Feet
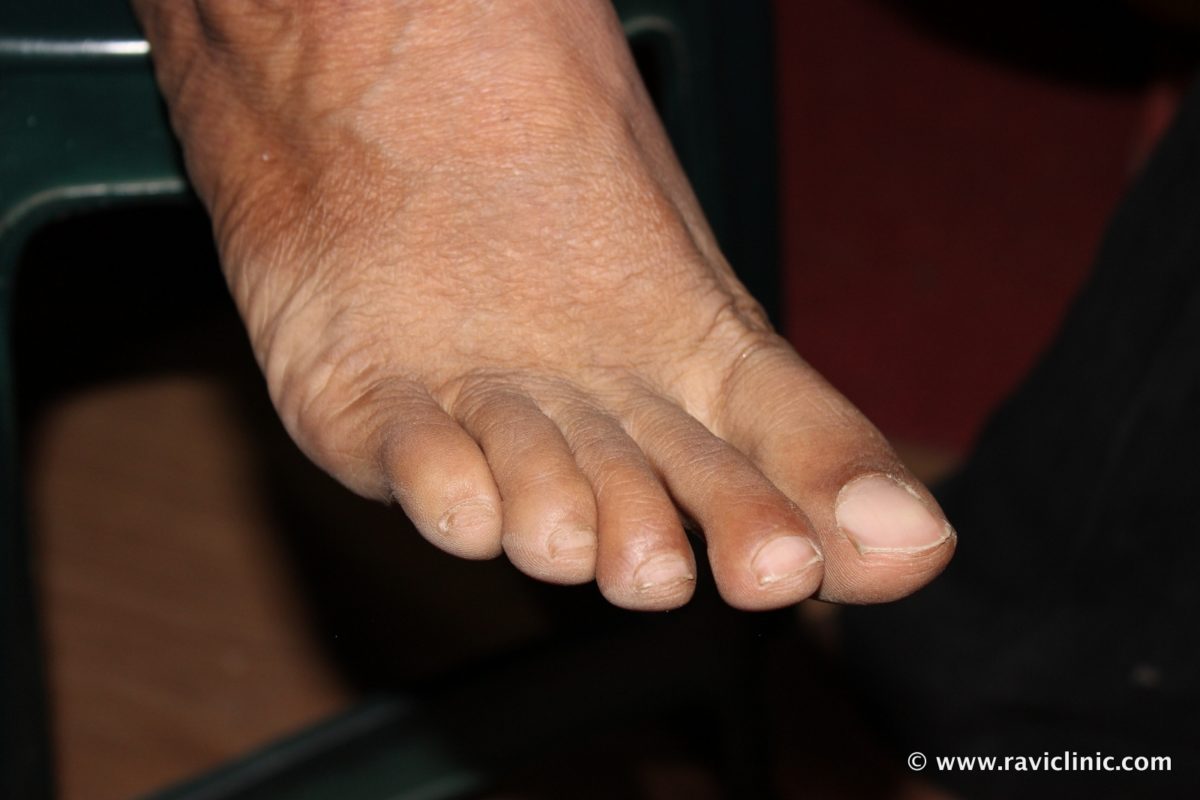
A case of Psoriasis at Feet Homeo Energy
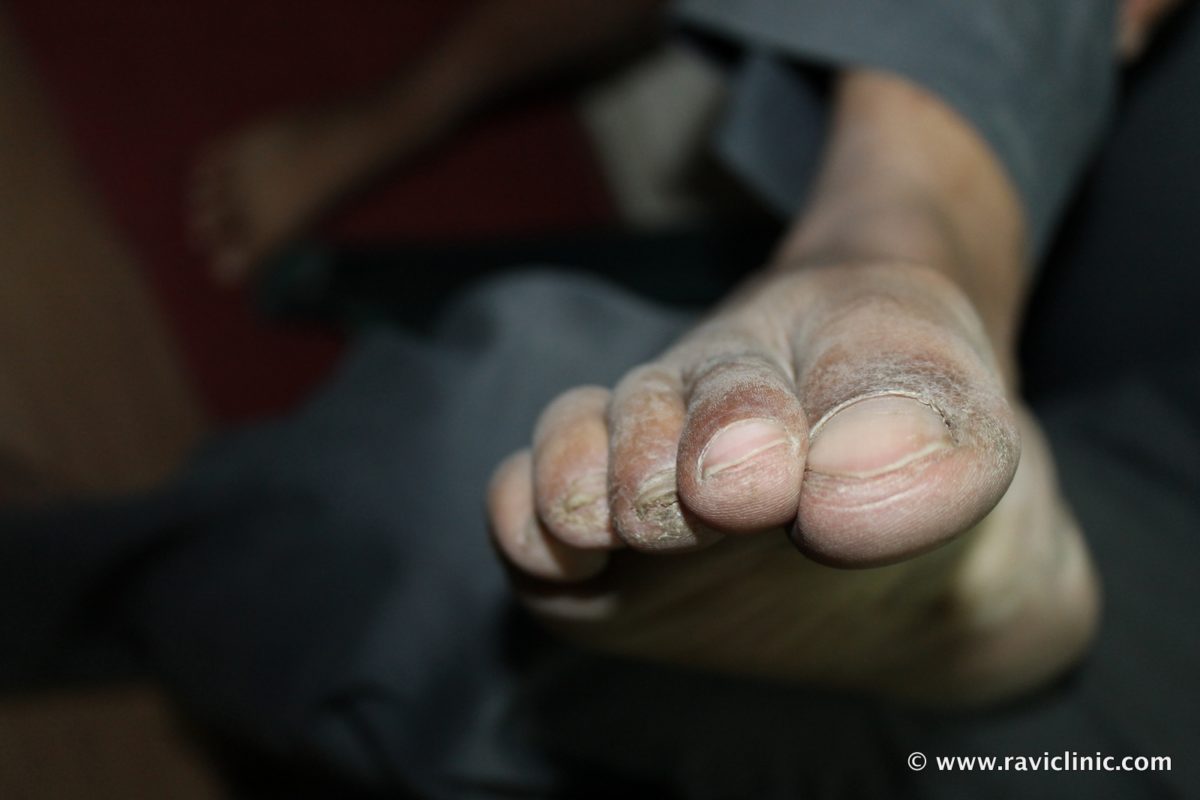
A case of Psoriasis at Feet Homeo Energy